wellbeing.humboldt.edu/data
This page is updated as report drafts and new data become available.
Understanding Student Physical and Mental Health Needs
The Health Need-Disparity Gap at Humboldt Overview (2 pages)
Why do health fees at Humboldt need to go even higher to meet students' needs? Get a quick understanding of the Physical/Mental Health Need-Capacity Disparity Humboldt students face and the four primary factors affecting cost and access, including systemic barriers and geographic location that dramatically affect student safety, quality of life, and retention.
Student Mental Health Need at Humboldt Executive Summary Presentation (24 Powerpoint Slides)
Presented to Associated Students on Feb 19, 2018 and the Faculty Senate Feb 20, 2018 these slides offer an overview and executive-level summary of existing services areas, the Physical/Mental Health Need-Capacity Disparity Humboldt students face that dramatically affect student safety, quality of life, and retention, and the Spring 2018 Health Fee adjustment consultation process. If you're interested in a presentation in your area, please contact us to schedule.
2017 Economic Analysis of Mental Health Services at Cal Poly Humboldt (2 pages)
This summary memo prepared by economist Daniel Eisenberg, Ph.D. on behalf of the Healthy Minds Network team (www.healthymindsnetwork.org) outlines (conservatively) loss in tuition revenue for Humboldt and reduction in total expected lifetime earnings of students incurred annually due the lack of capacity for additional mental health services.
2017 Healthy Minds Benchmarking Report on Prevalence of Mental Health Concerns among Humboldt students
Prevalence of Suicidal Behaviors and Prescription Medications Use Summary Graphics (2 pages)
This document presents graphically key findings from a 2016-2017 study (N=1717 out of a random sample of 4000 Humboldt students, a 43% response rate) on the prevalence of Mental Health Concerns at Humboldt, student needs, knowledge of services, and related help-seeking behaviors compared with over 100 universities nationally, and 10 peer institutions with similar enrollment, geographic region, and classification as Humboldt.
Descriptive Findings Report for Humboldt Data (23 Pages)
This report presents the results of a 2016-2017 study (N=1717 out of a random sample of 4000 Humboldt students, a 43% response rate) on the prevalence of Mental Health Concerns at Humboldt, student needs, knowledge of services, and related help-seeking behaviors. Among the most striking results are the findings that 61% of Humboldt students screen positive for some level of depression (compared with under 40% nationally), 68% mild or elevated anxiety, and 13% report suicidal ideation in the past year, with 9% reporting a plan. This all confirms or expands on other data reports including the ACHA National College Health Assessment (NCHA) survey and the National Survey of Student Engagement (NSSE).
Equity Data on Service Utilization by Racial/Ethnic Identity (8 Pages)
SH&WS takes an empirical approach to equity, believing it's not just enough to "be do gooders", we must also "do good". These summary graphs present the results of our examination of service provided in both initial visits and return visits broken down to compare under-represented and non-under represented groups. We also examined mental health-related items as part of our 2017 Healthy Minds study. Data show URG use SH&WS at a slightly lower rate than NURG initially, and that these differences are not attributable to stigma, knowledge of services, or need. Once students use our services URG and NURG return at roughly the same rates for follow-up visits.
2018 Humboldt Health Fee Adjustment Report and Five Year Strategic Plan for Student Health & Wellbeing Services
Please visit wellbeing.humboldt.edu/healthier-together to contribute between Feb 1 and March 9, 2018 and check back end of Spring 2018 for updated report information. This document will summary details of the empirically-informed rationale for needs, alternative ideas attempted or unavailable, and foreseeable services impact of insufficient health operations and facilities funding as well as the results of the 2018 campus-wide consultation process.
Student Health and Wellbeing Services Impact Retention and Student Success
Data on the impact of services on student success is critical. We also know poorly designed data collection and/or analysis can actually be worse than none if it leads to a firm belief in incorrect conclusions. Fortunately a number of quality, well-designed studies have been conducted over many years and the strong positive impact of health/counseling services on retention is settled science. Most of these studies also address key issues in research of this nature.
Key Research Considerations
Control group / selection bias:
It makes sense that individuals with lower food and security, for example, are more likely to use food pantry or other resources - individuals who are struggling on entry and have faced other barriers may be more likely to use health resources or CARE team services as well, and a well defined control group for equal risk is critical to measurement here or we risk concluding hospitals don't help, since they seem to be surrounded by people feeling sick.
Public Health vs. Individual impact:
Many of the health education and counseling services have impact at a community level. Does the mental health of the faculty members or RAs/ student leaders member who attends one of the I CAN HELP wellbeing ambassador training improve -- sometimes, but often it may be unaffected, actually, yet students on that individual's residence hall or in their class may be do better as a result. If we just measure the impact of individuals receiving services we don't capture the true impact. The same may be true when CAPS helps a student take time away from school to get treatment (negative impact on retention for that student ID) but the same action may keep 5 other people -- roommates, others on his/her sports team etc. - from transferring or failing because of the conflicts the student who left was at the center of. Effective health education can mean, in some case, fewer students receiving individual services with successful population-level interventions.
The Impact of Health and Wellbeing Services - Settled Science Research Summary
The utility of health and counseling services to improve student health and support retention is actually "settled science". That's in large part because this is actually a very well researched area, perhaps due in part to both the cost of investment in such services for universities and the number of trained researchers working in health and counseling centers. And, the research has been generally conclusive that 1) things like medical issues, depression, and anxiety, all reduce a students ability to succeed, 2) the services provided are adept at treating exactly these issues in the right dosage, and 3) the cost of services is greatly outweighed by the economic impact for universities from the resulting improvements in retention and even more powerfully by the lifelong contribution individuals who graduate make to society. Here are just a few examples of such existing knowledge:
Lee, Olson et al (2009). The effects of college counseling services on academic performance and retention. See article here: https://muse.jhu.edu/article/265820. Students receiving counseling services were 3.05 times more likely to stay enrolled in school compared to a non-counseling control group.
Porter, Shirley (2011). Personal Counselling at an Ontario Community College… Canadian Journal of Counselling and Psychotherapy / Revue canadienne de counseling et de psychothérapie ISSN 0826-3893 Vol. 45 No. 3 © 2011 Pages 208–219 First-year students who engaged in counseling had a 7.6% higher retention rate.
Schitzer, Alan et al (2018). Students With Mental Health Needs: College Counseling Experiences and Academic Success. In Journal of College Student Development, Jan-Feb 2018, Vol.59(1), pp. 3-20. View article here: https://muse.jhu.edu/article/684429. The number of counseling sessions was a significant positive predictor of cumulative GPA following counseling treatment AND was a positive predictor of whether or not students completed a degree within 6 years. For every 1-unit increase in the number of counseling sessions, the odds of degree completion increased by 5.1% Students with lower pre-college GPAs or psychologically high risk backgrounds = esp. important to target for counseling.
Bishop, Kyle. The Relationship Between Retention and College Counseling for High-Risk Students. View article here: http://web.a.ebscohost.com/ehost/detail/detail?vid=5&sid=bcbbbda9-b1df-4fcc-b2b6-8c8b1687a1e4%40sessionmgr4007&bdata=JnNpdGU9ZWhvc3QtbGl2ZQ%3d%3d#AN=118480352&db=eft. Low-risk students who used counseling services were retained at a significantly higher rate than high risk students who used counseling services.
Hjorth, Catherine et al (2016). Mental health and school dropout across educational levels and genders: a 4.8 year follow-up study. In BMC Publi9c Health, 2016, Vol. 16. Article here: https://link.springer.com/article/10.1186/s12889-016-3622-8 Showed that poor mental health was significantly associated to dropout among students in vocational and higher education. Males in higher education had 5x the risk of dropout when reporting poor mental health!
Dr. Daniel Eisenberg, an leading economist, has also done immense work in this domain - you can read more about his findings in papers like:
Eisenberg, Golberstein, & Hunt (2009), Mental Health and Academic Success in College, The B.E. Journal of Economic Analysis and Policy, 9(1).
Eisenberg, Daniel, Sarah Ketchen Lipson, and Julie Posselt. 2016. “Promoting Resilience, Retention, and Mental Health.” New Directions for Student Services 2016 (156): 87–95.
And on the website of the Healthy Minds Network at https://healthymindsnetwork.org/research/whitepapers-briefs/
Some whitepapers of specific interest include also:
Investing in Student Mental Health: Opportunities & Benefits for College Leadership
The Economic Case for Mental Health Services
Dr. Eisenberg's overall research over many years has found that mental health problems such as depression are associated with a two-fold increase in the risk of student departure [...] increasing the availability of services or preventive programs can reduce this risk and increase student retention [...and] mental health is correlated with higher satisfaction in college and higher reported likelihood of donating as a future graduate. And, for every 100 students who are given treatment for depression, as an example, you can avoid 6.48 drop-outs.
You can read more about the results of our 2017 study at Cal Poly Humboldt on our website at wellbeing.humboldt.edu/data and specifically review Dr. Eisenberg's memo on the economic analysis of mental health services at Humboldt. The CSU System is working with Dr. Eisenberg's team to conduct systematic research involving most or all of the 23-campus system using the HealthyMinds validated toolset this Spring 2020 and with Humboldt's Dr. Brian Mistler to prepare a CSU-wide analysis of the current state of mental health across the system which includes the impact on retention and university economics.
Student Health and Wellbeing Services ongoing Quality Improvement Data
Humboldt's Student Health and Wellbeing Services leadership and staff value ongoing quality improvement, and the use of data in decision making. Provided are a few examples of program evaluation conducted to evaluate and improve programs within our business unit in the past few years.
Laboratory Studies
Appropriate Laboratory Urine Protein and Sulfosalicylic Acid (SSA) Testing (Full Study Report PDF):
The goal of this study was to review current practice of confirming all abnormal dipstick urine protein’s with sulfosalicylic acid testing. Protein in urine can be the result of urological and nephrological disorders. But it can also be temporarily elevated by strenuous exercise, orthostatic proteinuria, dehydration, urinary tract infections and acute illness with fever. The protein test pad on the Siemens dipstick measures albumin. The sulfosalicylic acid test detects albumin, globulins and Bence-Jones proteins at low concentrations. The sulfosalicylic acid test is the differential screening urine protein test for monoclonal light chain diseases i.e. multiple myeloma or pancreatic transplants with anastomosis. The primary diagnostic procedure would be concomitant testing of all urine with both dipstick and sulfosalicylic acid. If albumin is not present with the dipstick, testing with sulfosalicylic acid will detect other proteins, including light chains. If albumin is present with the dipstick, testing with sulfosalicylic acid can only add additional information if the reaction is greater than the dipstick, indicating not only the presence of albumin but also globulins or Bence-Jones proteins. Our current practice of confirming positive dipstick with sulfosalicylic acid testing is screening for monoclonal light chain diseases.
Based on a review of our data and the literature, it was determined to discontinue confirming positive urine dipstick protein results with the SSA test. Our data show that the confirmatory test results agree well with the automated urinalysis result. Using a qualitative methodology to confirm another qualitative method duplicates work, increases costs and delays patient results.
Appropriate Laboratory Urine Specific Gravity and Refractometer Testing (Full Study Report PDF):
The goal of this study was to review current practice of confirming all dipstick urinalysis specific gravity’s ≥ 1.030 with a refractometer. The urine dipstick test is a screening test for a variety of metabolic disease processes. Normal specific gravity ranges from 1.001 – 1.035. A specific gravity of >1.023 in a random urine sample serves as good evidence that the concentrating ability is preserved. Kidneys lose concentration abilities in disease states such as diabetes insipidus where the urine has a fixed value of 1.010. Specific gravity is reported by dipstick method in increments of .005 from 1.000 to 1.030. The manufacturer states, “in general that the dipstick correlates within 0.005 with values obtained with the refractive index method.” Falsely elevated results may occur in the presence of moderate quantities of protein. The specific gravity dipstick test is not affected by the presence of radiopaque dyes as is the refractometer.
Based on a review of our data and the literature, we discontinued confirming specific gravity dipstick results ≥ 1.030. The urine dipstick is a screening test that can be completed in a matter of minutes at minimal expense with appropriate patient results. The timely results and reduced duplication of technologist testing services benefit the clinic and the patient. More accurate urine testing is available if the physician wants to pursue diagnosing metabolic diseases of the kidney.
Integration of Mental and Physical Health
Health Psychology Rotation (HPR) Pilot Study Fall 2017 (Full Study Report PDF):
The launch of the HPR may be better understood in the context of integrated health care, i.e., the integration of mental health care with physical health care. According to the Spring 2016 NCHA-ACHA report, university students identified stress, anxiety, sleep problems, depression, and cold/flu/sore throat as the top five health problems affecting their academic performance, which was almost identical to the reports of students at Cal Poly Humboldt who reported stress (41.1%), anxiety (33.1%), sleep problems (30.3%), depression (26.5%), and cold/flu/sore throat (22.5%) as their top (NCHA-ACHA, Spring 2016). Because of the high prevalence of mental health issues at primary care settings, integrated health care has shown to improve the quality of services, patients’ satisfaction, and cost-effectiveness in primary care settings (as cited in Peek et al., 2014). Some studies provided support for the better outcomes at college/university health care settings (Funderburk et al., 2012). A recent study reported that integrated health care of 9 university health centers was associated with lower primary care utilization of college students who have a mental health diagnosis when compared to standard (non-integrated) health care of 11 university health centers (Turner et al., 2108). Because of the clear needs for and benefits of integrated health care, the number of universities adopting integrated health care model appears to be on the rise.
According to the 2007 annual report by the Association for University and College Counseling Center Directors (AUCCCD, Rando et al., 2007), there were 16% of college counseling centers (n=57) that were “fully integrated” (i.e., offices are in the same building). In 2010, the AUCCCD annual survey was revised to ask the levels of integration of counseling services with health services. Twenty four percent of counseling centers (n=101) were reportedly “administratively integrated.” Similarly, in 2012, there were approximately 24% of counseling centers (n=98) “administratively integrated” (Mistler et al., 2012). However, in 2016, there were 31.7% of counseling centers (n=159) were “administratively integrated.” Of course, it is unclear whether the increase is statistically significant. In the 2017 annual report, the term, integrated, disappeared. Instead, a new word, collaboration, was used to describe how counseling centers worked with student health care centers. Fifty six percent of the counseling center directors (n=275) reported that they reported to the same supervisor as their medical counterparts did, indicating administrative integration, and 34.9% of the centers (n=125) shared the front desk staff. Although the 2017 AUCCCD survey tapped into various forms of collaboration, the use of HPR has not been reported.
In fact, the HPR may indicate a higher level of integrated health care, or collaboration, than simply reporting to the same supervisor or sharing the front desk. According to the Association of Psychology Postdoctoral and Internship Centers (APPIC), which takes charge of the national matching program that places psychology postdoctoral and doctoral trainees in full time residency training. As of April, 2018, there were 791 training sites participated in the national match for 2018. Among them, 591 centers/agencies described their sites as offering the HPR and 59 of them were university counseling centers offering training opportunities in health psychology. For the list of the 59 universities (Appendix A). Student Health and Well Being Services (SHWS) of Cal Poly Humboldt launched a health psychology rotation (HPR) in the fall 2017 semester, gearing toward an integrated model of college health care services. Multiple staff members from Counseling and Psychological Services (CAPS) and Student Health Services (SHC) were involved. The rotation model was ultimately replaced with a case manager model following the results of this pilot study.
Peer Education
We recently began implementation of a peer to peer model to provide asymptomatic STI screenings and birth control consults. By using a peer to peer model it was anticipated that medical staff would have more time to see more complex and acute issues and we would increase the number of students being screened for STI’s. We conducted a number of studies to evaluate the success of this program.
Humboldt Student Medical Services QI Re-Study Peer Health Educators in Clinic, Provider Follow-up Fall 2018 (Full Study Report PDF):
The purpose of this re-study is to evaluate how often a patient seen by a Peer Health Educator (PHE) subsequently needed to be seen by a provider and compare findings from fall 2017 with fall 2018
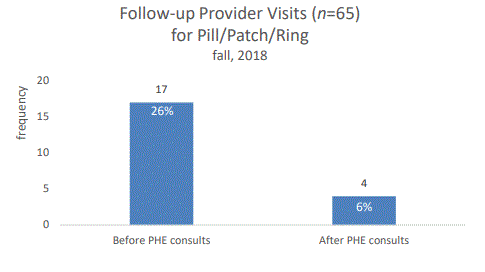
Humboldt Student Medical Services QI Study Peer Health Educators in Clinic, Pill/Patch/Ring Consults Fall 2018 (Full Study Report PDF):
Analysis showed that the most common reason a patient needed to follow-up with a provider after seeing a peer health educator (PHE) was for a pill, patch, or ring consult (38%). In the fall of 2018 PHEs were trained to provide pill, patch, or ring consults. The purpose of this study is to evaluate how effective these consults were in decreasing the need to be seen by a provider. As shown, before the PHE pill/patch/ring consults 26% of the provider follow up visits were for pill/patch/ring. This decreased to 6% after PHE consults started.
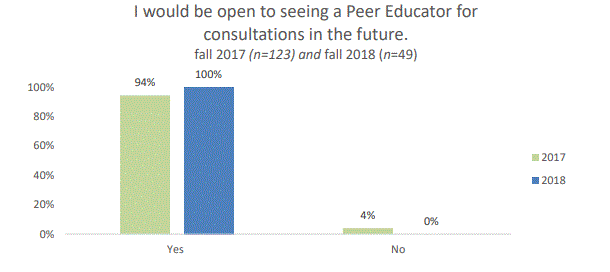
Humboldt Student Medical Services QI Re-Study Peer Health Educators in Clinic, Patient Satisfaction Fall 2018 (Full Study Report PDF):
College students are at high risk for sexually transmitted infections (STIs) and they are encouraged to get screened regularly. In 2016/2017 academic year, Humboldt Student Medical Services performed 2,019 screenings for STIs equating to 14% of all visits. In the fall of 2017 we implemented a peer to peer model to provide asymptomatic STI screenings and birth control consults. Evaluation of the program in 2017 showed it was effective and there was a high satisfaction rate among patients who participated in the program. In the fall of 2018 we had a new set of four peer heath educators (PHEs) who were trained to provide asymptomatic STI screenings and birth control consults in clinic. The purpose of this re-study is to evaluate patient satisfaction among participants of the PHE program in the fall of 2018 and compare it to the fall of 2017. We exceeded the performance goal of at least 90% of student participants being satisfied with the PHE program. While the findings from 2017 showed high levels of satisfaction, the numbers got even better in 2018.
Humboldt Student Medical Services QI Study Peer Health Educators in Clinic Demand, Utilization, and Cost Analysis Fall 2018 (Full Study Report PDF):
The purpose of this study is to evaluate the demand, utilization, and cost of the program during the fall 2018 semester. PHEs completed 387 patient visits during the fall 2018 semester. The only insurance the health center bills is Family Pact (FPACT) insurance. There were 364 PHE visits that were billed to FPACT for a total of $7,971.8. Additionally, FPACT reimburses for condoms ($15 for each bag) and blood draws ($3.60 for each blood draw). PHEs gave 155 bags of condoms and there were 214 FPACT blood draws and 6 non-FPACT blood draws. The total amount of PHE wages paid by the health center was $5,798.40 (some had work-study so the university paid part of wages). Overall, there was a net gain of $4,362 from the PHE program in the fall of 2018. This study shows that the PHE program is beneficial for meeting demand and freeing up providers for other types of visits, so we will continue the program.

